If you’ve ever woken up with a sharp, shooting pain travelling from your lower back down to your foot, you’ve likely asked yourself: Is this sciatica or just regular back pain? You’re not alone; millions of Americans face this exact confusion every year, and getting the diagnosis right is the first step toward effective relief. In many cases, people turn to medications like Aspadol tabs, which are used to treat moderate to severe acute and chronic pain, especially when discomfort begins to interfere with daily life. Both conditions can be debilitating, often leaving you wondering why your back hurts every day, while disrupting sleep, work, and overall quality of life. However, they are not the same—and treating them as if they are can sometimes make the problem worse.
This guide breaks down everything you need to know, including symptoms, causes, duration, and the most effective treatment options available—from prescription back pain medicines to modern approaches like tapentadol-based therapies.
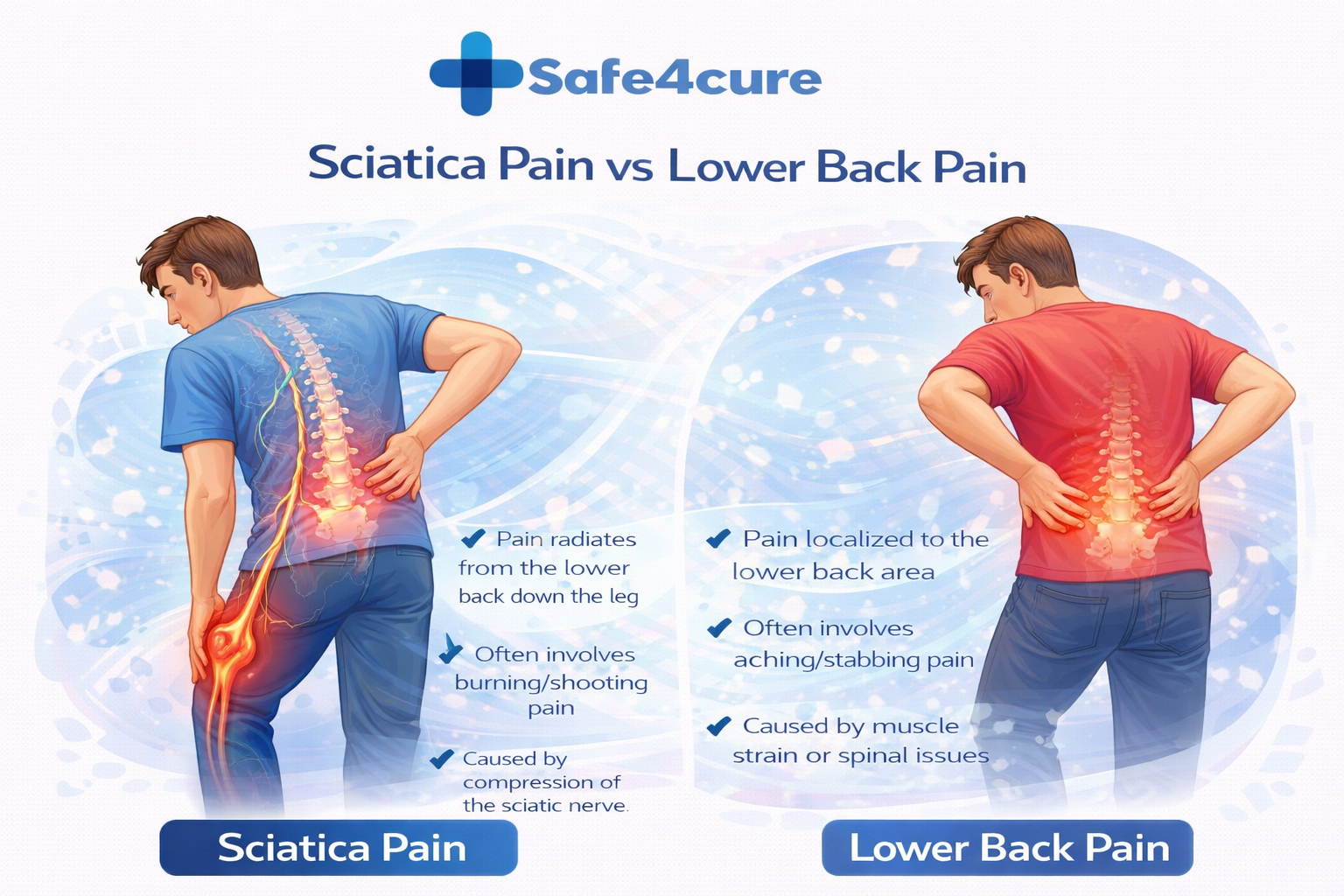
Sciatica vs. Lower Back Pain: The Core Difference
The most important distinction is this: lower back pain stays in the back, while sciatica travels. Sciatica is caused by compression or irritation of the sciatic nerve — the longest nerve in your body — which runs from your lower spine through your hips, buttocks, and down each leg.
Sciatica pain symptoms often include a burning or electric shock-like sensation that radiates down one leg, sometimes reaching as far as the toes. Regular lower back pain, on the other hand, is typically localized — felt as a dull ache, stiffness, or muscle tension confined to the lumbar region.
| Feature | Sciatica | General Lower Back Pain |
|---|---|---|
| Pain location | Lower back → buttock → leg → foot | Lower back only |
| Pain type | Sharp, burning, electric, shooting | Aching, dull, stiff, tight |
| One side or both | Usually one side | Can be both sides |
| Numbness / tingling | Common in leg or foot | Rare |
| Worsens when sitting | Yes, typically | Varies |
| Muscle weakness | Possible in leg | Uncommon |
Recognizing Sciatica Symptoms
The classic sciatica symptoms go beyond back pain. Look for these specific warning signs:
- Pain that radiates from the lower back through the left or right buttock and down the leg
- Tingling or numbness, especially in back left side pain or back right side pain that extends to the leg
- A feeling like an electric shock when you sneeze, cough, or sit for extended periods
- Weakness in the affected leg or foot
- Difficulty standing up after sitting
- In severe cases, loss of bladder or bowel control (seek emergency care immediately)
Does sciatica cause lower back pain? Yes — absolutely. In most sciatica cases, the lower back is the origin point of the pain before it travels downward. But having lower back pain alone does not mean you have sciatica. The traveling nerve pain is what distinguishes it.
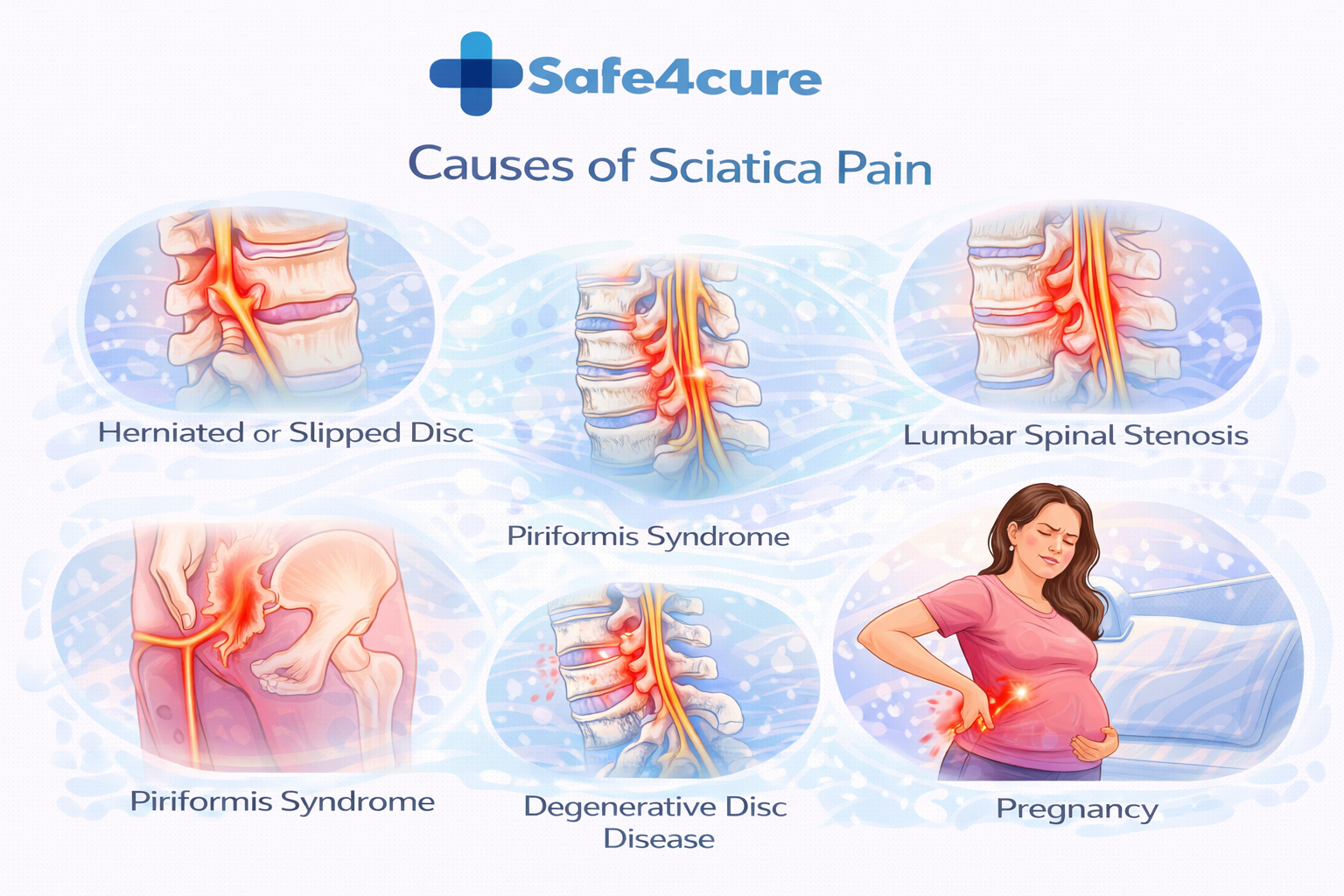
What Causes Sciatica Pain?
Understanding what causes sciatica pain helps explain why the right treatment matters so much. The most common culprits include:
1. Herniated or Slipped Disc
This is the number one cause in the US. When the soft cushion between spinal vertebrae bulges or ruptures, it can press directly on the sciatic nerve, triggering that characteristic shooting pain down the leg.
2. Lumbar Spinal Stenosis
As people age, the spinal canal can narrow — a condition common among Americans over 50. This narrowing compresses nerves, including the sciatic nerve, especially during walking or standing.
3. Piriformis Syndrome
The piriformis muscle, deep in the buttock, can spasm and irritate the sciatic nerve. This is common among runners and people who sit for long hours — a group that has grown significantly in the remote-work era.
4. Degenerative Disc Disease
Natural wear-and-tear on spinal discs over time can contribute to nerve compression, and it's one of the most frequent underlying causes of severe back pain in adults over 40.
5. Pregnancy
In the US, sciatica affects a notable portion of pregnant women, especially in the third trimester, as the expanding uterus puts pressure on the sciatic nerve.
How Long Does Sciatica Pain Last?
How long sciatica pain lasts depends largely on the underlying cause and how quickly treatment begins. Acute sciatica from a mild disc irritation may resolve in 4–6 weeks with rest, physical therapy, and anti-inflammatory care. However, chronic sciatica — especially when caused by structural issues like stenosis — can persist for months or even years without proper intervention.
In contrast, most episodes of non-specific lower back pain improve within 2–4 weeks. This is one reason proper diagnosis matters: if you treat sciatica like ordinary back pain, you may be managing it incorrectly for months.
Sciatica Pain Treatment & Lower Back Pain Relief
Treatment ranges from conservative home-based approaches to prescription medication for more severe cases. Here's what sciatica pain treatment typically looks like in the United States:
Conservative First-Line Treatment
For most patients, doctors start with physical therapy, targeted stretching (especially piriformis and hamstring stretches), ice/heat therapy, and over-the-counter NSAIDs. These steps provide meaningful sciatica pain relief and lower back pain relief for many people within weeks.
Interventional Options
When conservative care isn't enough, epidural steroid injections, nerve blocks, or chiropractic manipulation may be recommended. These options target the source of nerve compression directly.
Prescription Pain Medication
For moderate-to-severe cases — especially when severe back pain disrupts daily function — doctors may consider stronger back pain medicine or sciatica pain medicine. One option that has gained attention in pain management is tapentadol.
Tapentadol is a centrally-acting analgesic approved by the FDA for managing moderate to severe acute and chronic pain. It works through a dual mechanism: mu-opioid receptor agonism and norepinephrine reuptake inhibition. Branded as Nucynta (tapentadol brand name), it's considered part of the tapentadol CNS-acting drug class.
- Classified as a controlled substance (Schedule II) in the United States
- Belongs to the tapentadol class of opioids but with a distinct dual-action profile
- Available in immediate-release and extended-release formulations
- Sometimes prescribed for diabetic neuropathy pain, which shares features with nerve-based back pain
- Aspadol tabs are one of the internationally known tapentadol formulations used under medical supervision
It's important to understand that tapentadol and similar opioid-class medications are only prescribed when other treatments have not provided adequate relief. Because it is a controlled substance, it requires a valid prescription and careful medical supervision. Never self-medicate with these agents. Always consult a licensed physician or pain specialist before beginning any prescription regimen for the best pain medicine for sciatica or back pain.
Surgery (Last Resort)
A microdiscectomy or laminectomy may be recommended when there's significant nerve compression unresponsive to other treatments. The majority of sciatica patients, however, do not require surgery.
Final Thoughts
Both sciatica and lower back pain are among the most common pain conditions in the United States, and both deserve serious attention. The key takeaway is simple: location and character of pain matter. If your pain travels down your leg, involves numbness or tingling, and worsens when sitting, sciatica is a strong possibility.
Start with conservative care, stretching, physical therapy, and appropriate OTC sciatica pain medicine, but don't delay medical evaluation if symptoms are severe or persistent. For patients with complex or chronic pain, a physician may consider a full back pain treatment plan that includes prescription options, up to and including tapentadol-based CNS medications under careful medical supervision.